Gastrointestinal (digestive tract) care program
What is the Digestive System?
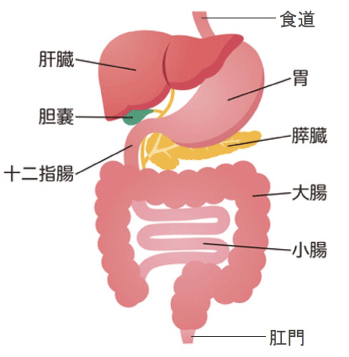
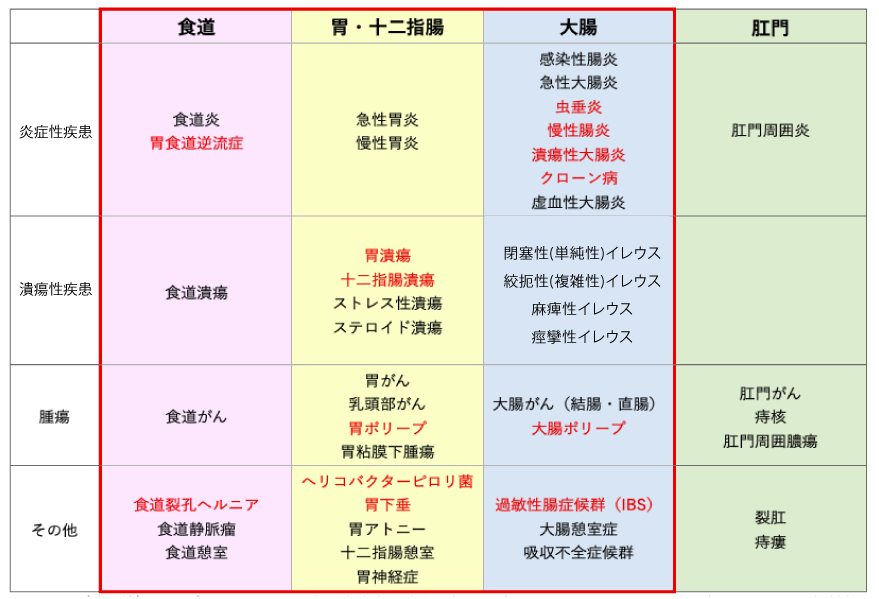
This Gastrointestinal (Digestive Tract) Care Program covers not only the diseases outlined in the red box on the chart but also Functional Dyspepsia (FD), which presents chronic epigastric pain, bloating, and discomfort without any apparent abnormality causing the symptoms.
What is Functional Dyspepsia (FD)?
Definition of Functional Dyspepsia
A condition where chronic epigastric pain, bloating, and other abdominal symptoms centered around the upper stomach occur despite the absence of organic, systemic, or metabolic disease as the cause.
Until now, such symptoms were often diagnosed as “chronic gastritis.” However, chronic gastritis refers to “inflammation in the stomach” (most often caused by Helicobacter pylori), but it has become clear that inflammation and symptoms are not necessarily related.
Therefore, around 1990, the American Gastroenterological Association introduced the concept of Functional Dyspepsia (FD).
Currently, reports suggest that the prevalence of functional dyspepsia is around 15%, making it a common condition. While it does not affect life expectancy, it impacts the quality of life (QOL) and requires appropriate treatment.
Causes
- When gastric and duodenal motility is impaired: This includes gastric emptying disorders and abnormal adaptive relaxation. Both delayed and excessively rapid gastric emptying can be related to symptoms, while impaired gastric adaptive relaxation is linked to early satiety.
Gastric Emptying: The process of moving food from the stomach to the duodenum.
Gastric Adaptive Relaxation: The stomach’s ability to expand and store food during meals. - When gastric and duodenal hypersensitivity occurs: Symptoms appear with less gastric distension compared to healthy individuals. Additionally, hypersensitivity to gastric acid and fat in the duodenum can trigger symptoms.
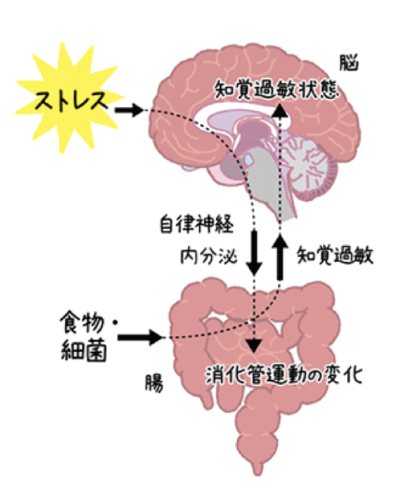
- Psychological factors (especially anxiety or history of abuse): The brain and gut are closely related. Anxiety, depression, or childhood abuse history may alter gastrointestinal motility and sensation.
- When gastric acid is the cause: Gastric acid can irritate the mucosa of the stomach and duodenum, affecting motility and sensitivity.
- When Helicobacter pylori infection is the cause: Symptoms may improve after H. pylori eradication.
- Genetic factors
- History of infectious gastroenteritis such as Salmonella infection
- Unhealthy lifestyle habits such as alcohol consumption, smoking, and poor sleep
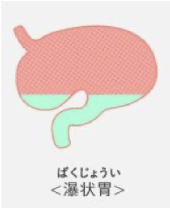
- Gastric morphology: Conditions like “hourglass stomach,” where the upper part of the stomach is expanded and deformed, may be related to symptoms.
Examinations & Diagnosis
To rule out diseases such as gastric cancer, gastric ulcers, or duodenal ulcers, an endoscopy of the stomach, a Helicobacter pylori test, and if necessary, blood tests, ultrasound, and abdominal CT scans are conducted.
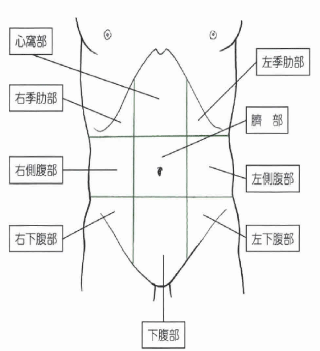
・Presence of chronic stomach pain or bloating symptoms.
※ Medically, this includes postprandial fullness, early satiety, epigastric pain, and epigastric burning sensation.
・No presence of diseases such as gastric cancer or gastric ulcers detected by endoscopy.
General Treatment
The main triggers for abnormalities are gastric movement and gastric acid. If the process of moving food from the stomach to the duodenum does not work well, symptoms such as bloating and pain may occur. For improvement, gastrointestinal motility improving drugs are used. Additionally, when gastric acid secretion causes pain or when excess gastric acid flows into the duodenum, causing nausea, acid secretion inhibitors are used to suppress the gastric acid secretion.
This occurs when there is hypersensitivity to various stimuli. It is difficult to suppress an overly sensitive brain state, but some anti-anxiety drugs and antidepressants have been shown to improve FD symptoms. Furthermore, herbal medicine has been shown to improve FD symptoms by improving stomach movement or increasing appetite, although there is not enough evidence to fully support this.
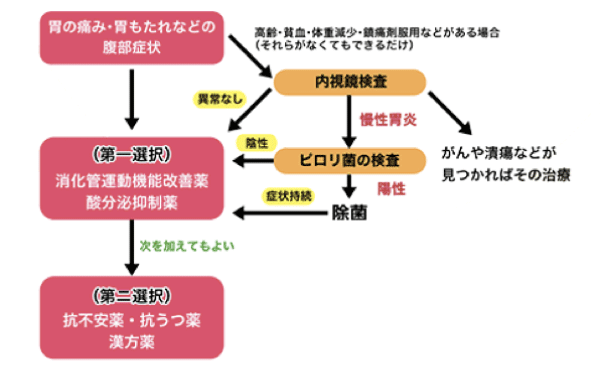
Treatment is done by consulting with the patient and the doctor to test which medications work best, and sometimes using a combination of medications with different effects. Under the guidance of a reliable doctor, proper medication, along with lifestyle and dietary improvements, is essential.
Cure Rate and Associated Diseases
Irritable Bowel Syndrome (IBS)
Irritable Bowel Syndrome (IBS)
It is a disease suspected when abdominal pain and discomfort are accompanied by bowel irregularities, such as constipation or diarrhea (in terms of frequency and shape), that last for several months or more. It is assumed that there are no organic diseases like tumors or inflammation in the large intestine.
Causes
The cause of IBS is unknown. However, it is known that after an infectious gastroenteritis caused by bacteria or viruses, people are more likely to develop IBS upon recovery.
Examination and Diagnosis
However, to confirm that there are no serious conditions like colon cancer or inflammatory bowel disease, or if the symptoms are severe or do not improve with treatment, tests such as blood tests, abdominal ultrasound, abdominal CT scans, fecal occult blood tests, colonoscopy, and colon contrast radiography may be conducted.
Type Classification
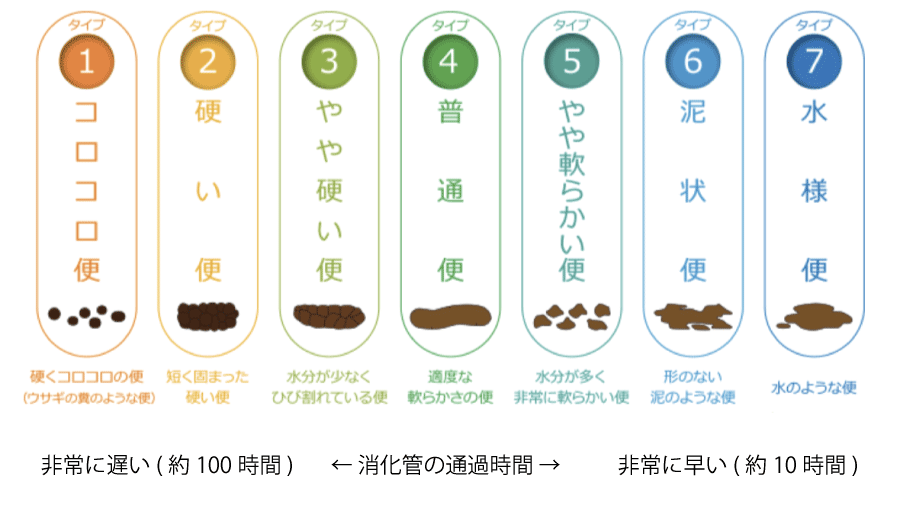
The Bristol Stool Form Scale is used to classify the stool form and frequency into the following 4 types:
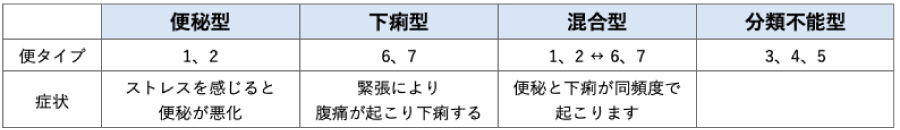
General Treatment Methods
Moderate exercise is also expected to help alleviate symptoms. Aim for sustainable levels of physical activity.
Precautions
Abdominal pain and bowel irregularities tend to improve with age, and the likelihood of developing a disease is lower. However, the type of bowel irregularity may change. Compared to healthy individuals, those who experience stomach pain, bloating (functional dyspepsia), heartburn, and acid reflux (gastroesophageal reflux disease) are more than twice as likely to have these symptoms. Additionally, depression and anxiety are more likely to co-occur, and the impact on daily life may be more significant.
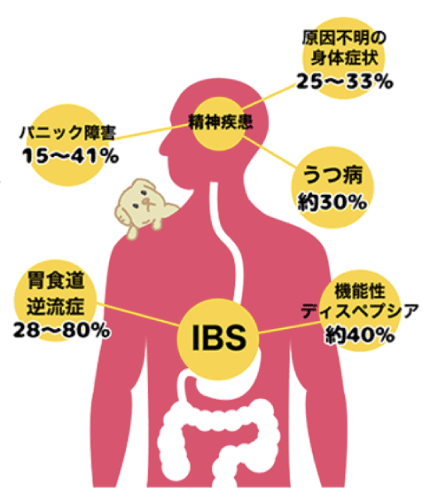
Prevention
Currently, there are no studies proving IBS can be prevented, but some risk factors for IBS are known. Among these, the risk factors that can be reduced by individuals include stress, depressive tendencies, excessive concern about physical abnormalities, and smoking.
Getting adequate sleep, maintaining a regular lifestyle, and practicing relaxation methods suited to you—without relying on alcohol or tobacco—are helpful. Additionally, making dietary adjustments, exercising, and consuming probiotics may help prevent IBS.
Interventions Available Only at Medical Japan
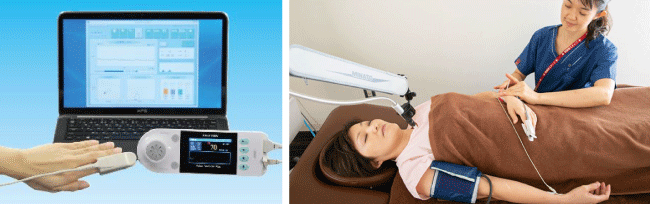
Autonomic Nervous System and Peripheral Blood Flow Diagnosis
While providing dietary and lifestyle modification advice to improve symptoms, we also check the status of the autonomic nervous system, which is influenced by stress, and the blood flow to internal organs. Depending on the degree and duration of stress, it is possible to identify whether the problem lies in the sympathetic or parasympathetic nervous system, and what type of care is required.
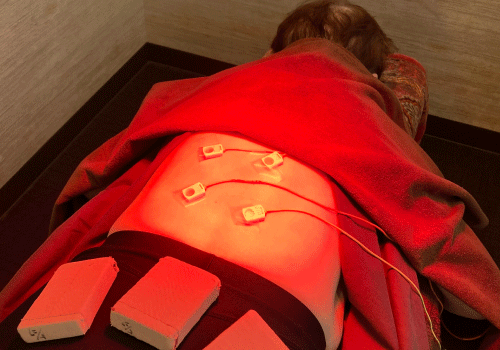
Improving Internal Organ Blood Flow: Intervention Example Using Moxibustion
Moxibustion has been confirmed to improve the blood flow to internal organs and activate the digestive system and metabolism. For the elderly, the decline in basal metabolism and indigestion can be major obstacles to dieting, but these issues can be improved through moxibustion.
This patient had been suffering from chronic indigestion and constipation. By regularly performing moxibustion, blood flow to the internal organs improved, the digestive system became more active, and bowel movements became smoother. Furthermore, with improved metabolism, the patient experienced weight loss. This is an example of successfully managing weight healthily with a diet plan incorporating moxibustion.
Gastrointestinal Care Breathing Exercises
We teach exercises and breathing techniques that can be practiced daily. Through proper instruction by medical professionals with national qualifications, we strive to improve symptoms and prevent recurrence.